This suggests that if the variables are reduced and controlled, a PRP preparation and application protocol can be developed leading to PRP inducing reliable, complete, and long-term pain relief.” The best explanation for the variability in PRP analgesic efficacy is the failure during PRP preparation and application to take into account variables that can increase or eliminate its analgesic capabilities. The variability in PRP efficacy raises the question of whether PRP actually has an analgesic capacity, and if so, can that capacity be made consistent and maximized. Variability in treatment can lead to failure: “Despite great variability in pain outcomes, the application of autologous platelet-rich plasma (PRP) has become increasingly popular in attempts to reduce chronic pain.This was a recent study published in the Journal of pain research.( 3) It hits upon some good points that describe how PRP works and when PRP may not work. It usually takes time and numerous treatments / injections to rebuild the soft tissue of that hip. Your hip osteoarthritis did not occur overnight, it is the result of a slow degenerative process. In some research and in many doctor’s offices PRP is treated somewhat like a cortisone injection where one quick injection is considered the treatment. In our opinion, regenerative medicine results are best seen when multiple PRP injections are given. Larger future trials including a placebo group are required to further evaluate these promising results.” Research into 2021 continues to suggest the effectiveness of PRP for hip osteoarthritis.īefore we look at other research that supports the use of PRP for hip osteoarthritis treatments, I want to explain the variations someone researching or getting this treatment may experience. In 2018 a study ( 2 ) from the United Kingdom suggested: “Literature to date concludes that intra-articular platelet-rich plasma injections of the hip, performed under ultrasound guidance to treat hip osteoarthritis, are well tolerated and potentially efficacious in delivering long-term and clinically significant pain reduction and functional improvement in patients with hip osteoarthritis. Time tested interventions such as arthroplasty have shown good results and still have a major role to play but newer, regenerative approaches have the potential to effectively delay or reduce the requirement for such invasive procedures.” Here is what the study said: “Orthopedic surgeons are at an exciting crossroads in medicine, where hip biologic therapies are evolving and increasingly available. Research on PRP for Hip OsteoarthritisĪ February 2021 study ( 1) gives a very optimistic assessment that the days of hip replacement may be coming to an end. It is important to note that this treatment will not help everyone. The collected platelets are then injected back into the injured area to stimulate healing and regeneration. Platelet-Rich Plasma therapy is part of a group of treatments that come under the term “regenerative medicine.” PRP treatments involve collecting a small amount of your blood and spinning it in a centrifuge to separate the platelets from the red cells. Someone who needs to get back to work or not lose time from a physically demanding job will need a different program than a retired person with limited activity. For instance, a patient who wants to climb a mountain in a few months will need a different treatment program than someone who simply wants to walk up a flight of stairs without loss of stability and pain. How do we decide which treatment will be best? Many factors. Following the consultation we sit down with the patient and present our recommendations for their hip pain treatments. When a patient comes into our office, the realistic expectation of effectiveness of treatment is confirmed by a physical examination and a patient history. 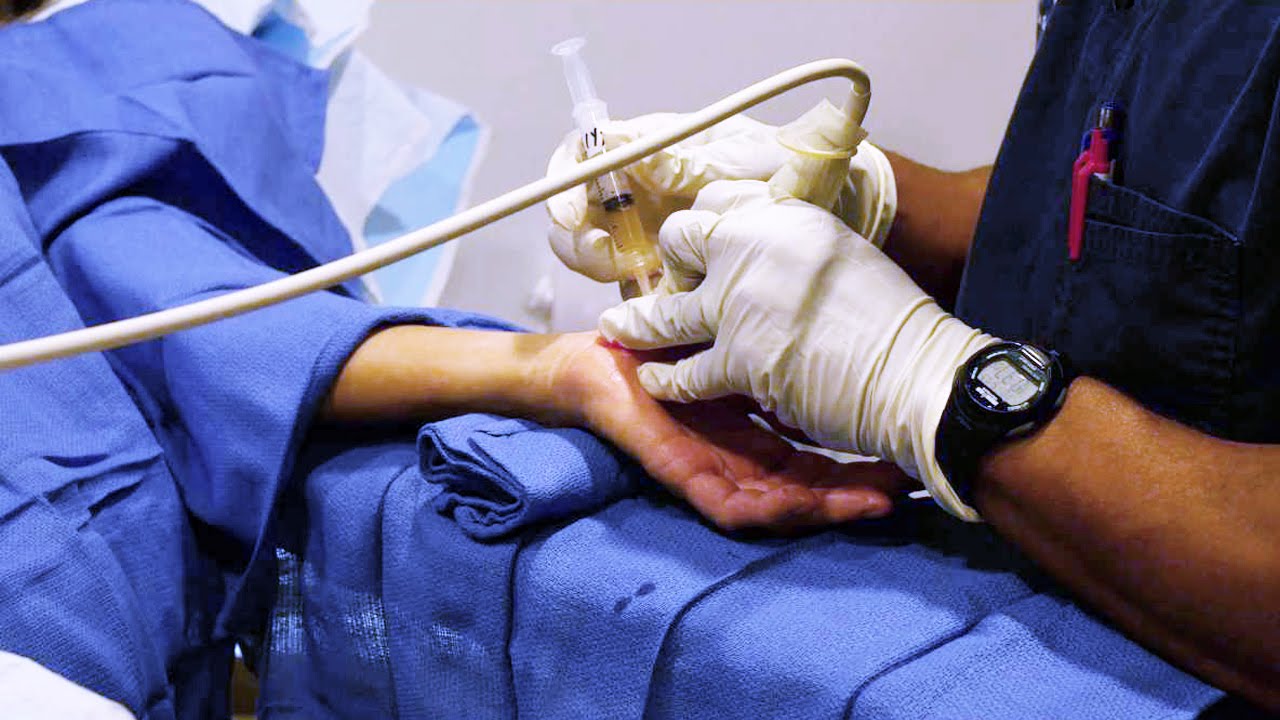
Bone marrow derived stem cells and Platelet Rich Plasma injections have been seen as effective and reliable treatments for the patient with hip osteoarthritis.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
